
Health


Share
Published 12:27 8 May 2022 BST
Updated 12:35 4 May 2022 BST

Explore more on these topics:
 Fatigue, 'brain fog', problems recalling words, sleep disturbances, anxiety and even post-traumatic stress disorder (PTSD) were some of the lasting cognitive and mental health problems that scientists said Covid patients can experience months after infection.
They found this by analysing data from 46 people who received in-hospital care - either on the ward or in intensive care units - for Covid, 16 of whom experienced enough viral infection that they had to be put on mechanical ventilation.
Patients underwent "detailed computerised cognitive assessment alongside scales measuring anxiety, depression and post-traumatic stress disorder under supervised conditions," the research article stated. Analysis revealed that Covid survivors were less accurate and had slower response times when compared with the general population - a difference which was still detectable six months later.
[caption id="attachment_333449" align="alignnone" width="2048"]
Fatigue, 'brain fog', problems recalling words, sleep disturbances, anxiety and even post-traumatic stress disorder (PTSD) were some of the lasting cognitive and mental health problems that scientists said Covid patients can experience months after infection.
They found this by analysing data from 46 people who received in-hospital care - either on the ward or in intensive care units - for Covid, 16 of whom experienced enough viral infection that they had to be put on mechanical ventilation.
Patients underwent "detailed computerised cognitive assessment alongside scales measuring anxiety, depression and post-traumatic stress disorder under supervised conditions," the research article stated. Analysis revealed that Covid survivors were less accurate and had slower response times when compared with the general population - a difference which was still detectable six months later.
[caption id="attachment_333449" align="alignnone" width="2048"]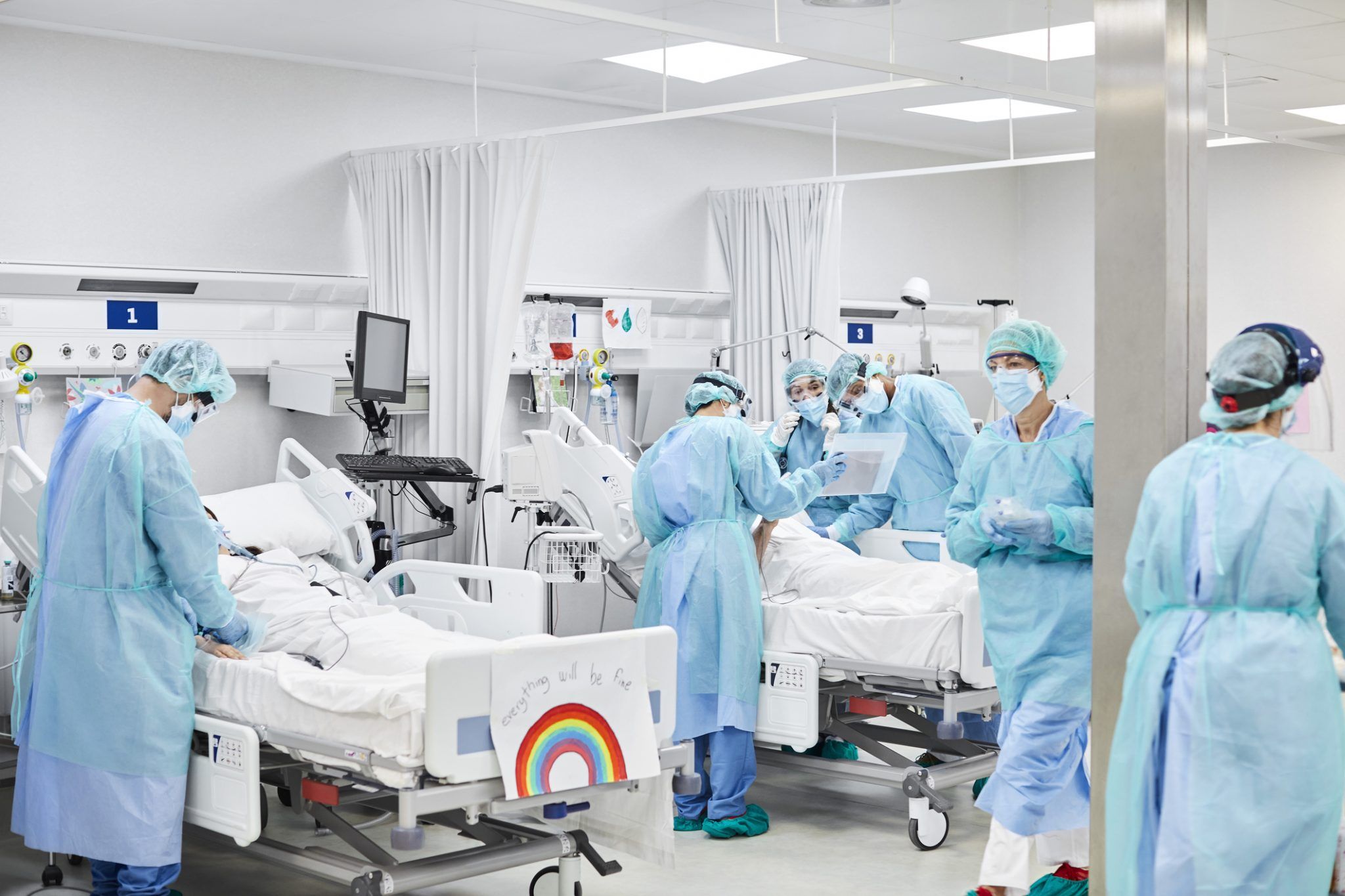 Many patients with severe Covid required ventilation [/caption]
The impacts were strongest amongst those who required mechanical ventilation but even patients who weren't sick enough to be hospitalised could have tell-tale signs of mild impairment.
Verbal analogical reasoning was an area that those who had overcome severe covid illness scored especially poorly on when completing tasks. In addition, survivors also found it difficult to find the right words and experienced slower processing speeds.
The study's senior author, Professor David Menon from the Division of Anaesthesia at the University of Cambridge explained: "Cognitive impairment is common to a wide range of neurological disorders, including dementia, and even routine ageing, but the patterns we saw – the cognitive 'fingerprint' of Covid-19 – was distinct from all of these."
There are several factors that could cause the cognitive deficits, researchers said.
Many patients with severe Covid required ventilation [/caption]
The impacts were strongest amongst those who required mechanical ventilation but even patients who weren't sick enough to be hospitalised could have tell-tale signs of mild impairment.
Verbal analogical reasoning was an area that those who had overcome severe covid illness scored especially poorly on when completing tasks. In addition, survivors also found it difficult to find the right words and experienced slower processing speeds.
The study's senior author, Professor David Menon from the Division of Anaesthesia at the University of Cambridge explained: "Cognitive impairment is common to a wide range of neurological disorders, including dementia, and even routine ageing, but the patterns we saw – the cognitive 'fingerprint' of Covid-19 – was distinct from all of these."
There are several factors that could cause the cognitive deficits, researchers said.
 Direct viral infection is possible culprit however it's unlikely to be a major cause. In fact, researchers found that it is more likely that a combination of factors result in this impact - these include inadequate oxygen or blood supply to the brain, blockage of large or small blood vessels due to clotting and microscopic bleeds.
That said, emerging evidence reveals that the body's own inflammatory response and immune system could cause key damage.
Patient improvement was gradual at best - and for some, researchers predict that they might never properly recover.
Professor Menon said: "We followed some patients up as late as ten months after their acute infection, so were able to see a very slow improvement. While this was not statistically significant, it is at least heading in the right direction, but it is very possible that some of these individuals will never fully recover."
Direct viral infection is possible culprit however it's unlikely to be a major cause. In fact, researchers found that it is more likely that a combination of factors result in this impact - these include inadequate oxygen or blood supply to the brain, blockage of large or small blood vessels due to clotting and microscopic bleeds.
That said, emerging evidence reveals that the body's own inflammatory response and immune system could cause key damage.
Patient improvement was gradual at best - and for some, researchers predict that they might never properly recover.
Professor Menon said: "We followed some patients up as late as ten months after their acute infection, so were able to see a very slow improvement. While this was not statistically significant, it is at least heading in the right direction, but it is very possible that some of these individuals will never fully recover."What’s the Story with Rosacea? Expert shares what you really need to know
May is Rosacea Awareness Month May is Rosacea Awareness Month, but what do we really know about the skin condition? Known as the ‘Celtic Curse,’ the condition reportedly affects 10% to 12% of the population in Ireland, but many of us are guilty of brushing it off as ‘just redness.’ Dr. Edel Woods recently spoke […]
Health
1 day ago
What is PCOS and why has it been renamed?
Polycystic ovary syndrome (PCOS) impacts one in ten women in Ireland. You may have heard that polycystic ovary syndrome (PCOS) has officially been renamed. This comes after a 14 year battle, and a global push to improve diagnosis and treatment of the condition. It will now be known as polyendocrine metabolic ovarian syndrome (PMOS). The […]
Health
1 week ago
Health
How to tell you’re having a heart attack as Patrick Muldoon dies aged 57
Health